Laparoscopic Needle Drivers

Needle drivers, or needle holders, are used to grasp and manipulate needles to enable free-hand suturing of wounds or surgical incisions within the body during laparoscopic procedures. Surgical needle drivers have been in widespread use for little over a century. Prior to this, needles were large enough to be manipulated by hand, and any instruments that were developed to assist with suturing often had more in common with the tools of tailors, sail-makers or leatherworkers than with the surgical instruments of today.
The tip must transmit appropriate pressure

Belonging to the same family of instruments as pivoting or spring forceps, needle drivers for use in open surgical procedures generally have ringed handles for pincer-like operation using the thumb and one or more fingers, and are available in a wide range of lengths, sizes and styles, to suit many different types of needle . Needle control and performance is determined by the stability of the needle within the driver . Historically this has required the instrument to be matched to the needle size. Conversely, the range of needles and instruments available for use in minimally invasive procedures is much smaller, limited by the necessity for needle and driver to fit through laparoscopic access ports that are typically only 5mm in diameter, as well as the need to minimise the number of times instruments are moved in and out of the body during a procedure.
What are the design elements of a laparoscopic needle driver?
Laparoscopic needle drivers typically comprise a long narrow shaft, with a handle at one end and a set of hinged jaws at the other. The shaft is made of surgical steel with an outer layer of non-conductive plastic or silicone. Jaws are generally made of tungsten carbide and may have additional coatings applied to improve grip. Instruments are available in a range of different lengths, with 30 to 35 cm being the most common. Different lengths of jaw are also available, and devices may be reusable or disposable.
How do Needle Drivers differ from other laparoscopic instruments?
Unlike the handles of laparoscopic instruments used for grasping or cutting actions, which tend to be located at right angles to the shaft, needle driver handles are usually of a straight axial design that places the needle directly in line with the surgeon’s hand to allow greater manoeuvrability and a more natural motion of the wrist when suturing. Various designs are available, but generally the jaws of the instrument are operated by means of an ergonomic spring-loaded palm grip on the handle. The grip is squeezed to open the jaws and released to close them.
The anatomy of the surgical suturing needle
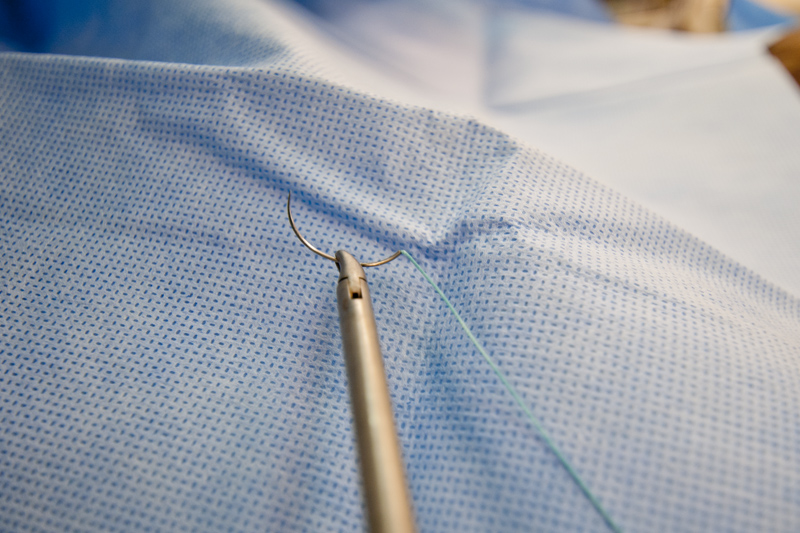
The needle is secured firmly in the jaws of the instrument by means of a ratcheted locking mechanism located in the handle. One of the most important considerations is that the release mechanism be easy to operate, as the surgeon must grasp and release the needle repeatedly whilst suturing. The position of the quick-release mechanism on the handle and the number of teeth on the ratchet are both factors in determining ease of use. Some designs also include a spring that can be adjusted to enable precise tensioning of the jaws on a variety of needle diameters.
What are the general categories of laparoscopic needle drivers?
Needle driver jaws fall into one of four main categories: straight, curved left, curved right and self-righting. Straight jaws sit in line with the shaft of the instrument. Curved jaws are angled to the left or right at approximately 45o to the shaft. When a needle is grasped in the flat jaws of a standard needle driver , it remains in the position in which it was grasped. This may then require the surgeon to rotate the needle driver up to 180o or to use a second instrument to move the needle into the required position within the jaws of the needle driver . Self-righting needle drivers attempt to address this issue by forcing the needle into a fixed position at either 90o or 45o to the shaft, depending on the instrument. This can be achieved using a set of jaws comprising a convex and corresponding concave jaw, designed to fit precisely the curved shape of the needle , forcing it into position. Other designs make use of interlocking protrusions on the upper and lower jaws to guide the needle into place when the jaws are closed. The use of self-righting needle drivers is limited by the fact that the instrument cannot usually be used to grasp the suture, as it may damage the material. Additionally, many surgeons prefer to have manual control over the angle of the needle within the instrument, in order to achieve optimal positioning for a given stitch.
What are the differences between the jaws of a needle holder?
Jaws can be double-action or single-action, with the latter being the more common. Tips are usually tapered to offer improved visibility at the suture site. The inner surface of the jaws may be coated with diamond or profiled with cross-serrated ribbing for a secure grip. The edges of the jaws should be rounded to prevent damage to the suture material. Some instruments include an integral knot pusher, consisting of a notch at the tip of the device that can be used to drive an externally tied knot into the body cavity. Other devices incorporate a suture cutting blade located close to the hinged joint such that it is protected during normal usage. More recently, needle drivers with an articulating tip that can be controlled by the angling the instrument’s handle are now available. Such devices theoretically offer greater manoeuvrability and efficiency when compared to non-articulating types, but have a steeper learning curve.
How does a surgeon decide which instrument to use?
Several different needle holders may be used in a given procedure, depending on the procedure and the surgeon’s preference. However, an instrument should ideally provide the surgeon with proper control over a range of different types and thicknesses of suturing material, such that the same instrument may be used to suture both course and fine tissue. Laparoscopic suturing requires skill and dexterity; the surgeon has an extremely restricted space in which to manoeuvre the needle , and the two-dimensional view of the operating site provided by the laparoscope affords limited depth perception. Certain types of suturing materials can be particularly difficult to work with due to their stiffness and tendency to resist deformation, and forming the slip-knots required to close wounds and surgical incisions requires great skill. It is common for the surgeon to operate the needle driver in tandem with a grasper, tissue forceps or second needle driver in order to achieve an efficient suturing technique. Specific instruments are also available to assist with suturing, including knot pushers and needle forceps.
A multitude of robotic needle drivers