Robotic Nerve Grafting
Video assisted thoracoscopic sympathectomy is an accepted therapy for hyperhydrosis that is socially debilitating. This procedure usually has excellent outcomes, but does have a small subset of patients who develop compensatory sweating so severe that it becomes more problematic than the initial hyperhydrosis. These patients suffer with pronounced sweating of the trunk, abdomen, buttocks and thighs.
The incidence is low given improved surgical technique and patient selection. A subset of these patients is so dissatisfied that they are candidates for a reversal procedure. Previous reversal procedures have required a traditional thoracotomy to allow reconstruction of the sympathetic chain with a sural nerve graft. Our experimental aim was to test the feasibility of using the Da Vinci Robot to perform a minimally invasive thoracic microsurgical reconstruction of the sympathetic chain. Robotic intercostal nerve grafting for reversal of thoracic sympathectomy is a procedure that is technically feasible. The device's tremor filtration, dexterity in small spaces and high magnification camera make this a viable minimally invasive option to reconstruct the sympathetic chain. The principles of neural microsurgery are also maintained with this approach. Future studies will evaluate the efficacy of the nerve graft in a survival model with functional nerve conduction studies and histologic evaluation.
Hyperhidrosis Reversal for Compensatory Sweating
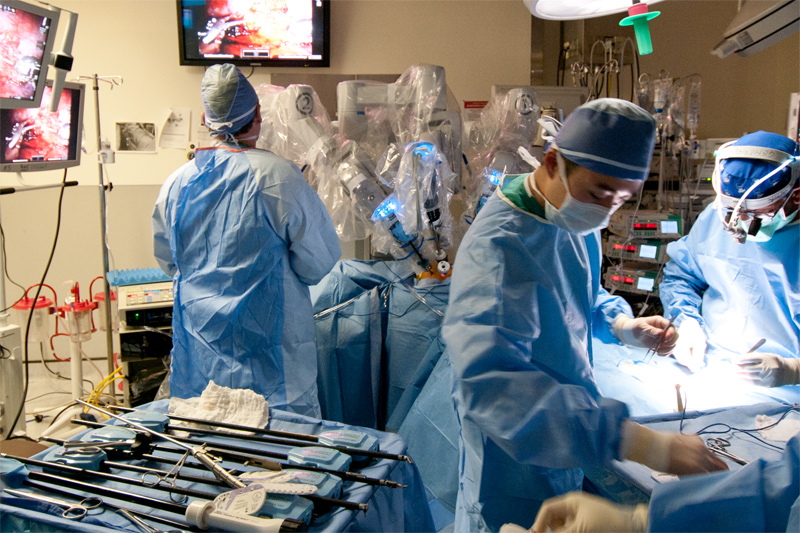 The first robotic sympathetic nerve grafting in the world was performed at St. Luke's – Roosevelt. This technique combines the advantages of neurosurgical microsurgery with the minimally invasive capabilities and motion scaling of robotics. All patients are studied both before and after the operation in order to best evaluate the potential of the technique.
The first robotic sympathetic nerve grafting in the world was performed at St. Luke's – Roosevelt. This technique combines the advantages of neurosurgical microsurgery with the minimally invasive capabilities and motion scaling of robotics. All patients are studied both before and after the operation in order to best evaluate the potential of the technique.Video Image Overlay in Robotic Surgery
A hypothetical advantage of the DaVinci Robot is that it is an information console that can incorporate various data sources to best serve the operating surgeon. Image overlay has thus far been explored only in virtual environments. The aim of our study was to evaluate the feasibility of real-time fluoroscopic overlay in a laboratory model and to provide a workable technique that could be readily incorporated into procedures using current technology.
Video Overlay
 Limitations of fluoroscopic disparity are demonstrated in bench models attempting visual and radiographic overlay.
Limitations of fluoroscopic disparity are demonstrated in bench models attempting visual and radiographic overlay.Image alignment can be achieved in a laboratory model only in one plane. A 0 degree laparoscope exactly aligned with the collimator causes a fluoroscopic blind-spot. Moreover, disparity in the superimposition of the robotic instruments increases in a uniform manner as the distances from the collimator changes, negating intraoperative overlay with current technology. A picture-in-picture manner of real-time fluoroscopic and video imaging with a 30 degree laparoscope proved optimal. Real time fluoroscopic and video overlay are not possible secondary to disparity in multiple planes. A picture-in-picture fluoroscopic/video combination was very helpful and will be used in future procedures.
Fluoroscopic Localization Applied to Robotic Lung Cancer
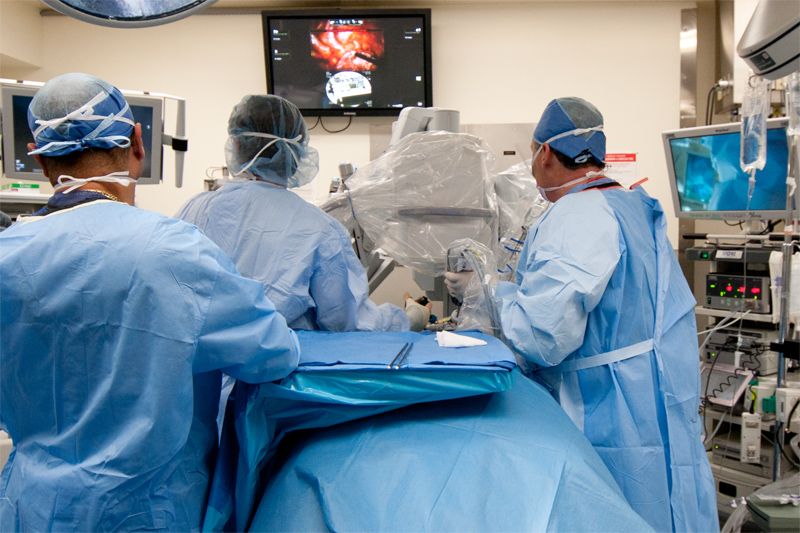 There are situations where early lung cancer tumors can be resected without requiring a formal lobectomy. While tumors on the outside of the lung can sometimes be seen with standard video scopes, tumors that are buried deep inside the lung require other options. An evolution of the initial lab project of fluoroscopic overlay is applying interventional placed markers and then robotic assisted thoracoscopic resection. The monitor in the center demonstrates the thoracoscopic view and then the fluoroscopic image on the bottom.
There are situations where early lung cancer tumors can be resected without requiring a formal lobectomy. While tumors on the outside of the lung can sometimes be seen with standard video scopes, tumors that are buried deep inside the lung require other options. An evolution of the initial lab project of fluoroscopic overlay is applying interventional placed markers and then robotic assisted thoracoscopic resection. The monitor in the center demonstrates the thoracoscopic view and then the fluoroscopic image on the bottom.

 Robotic nerve grafting is shown being performed in an animal model. The procedure has hypothetical benefit for the reversal of sympathectomy performed or hyperhidrosis
Robotic nerve grafting is shown being performed in an animal model. The procedure has hypothetical benefit for the reversal of sympathectomy performed or hyperhidrosis