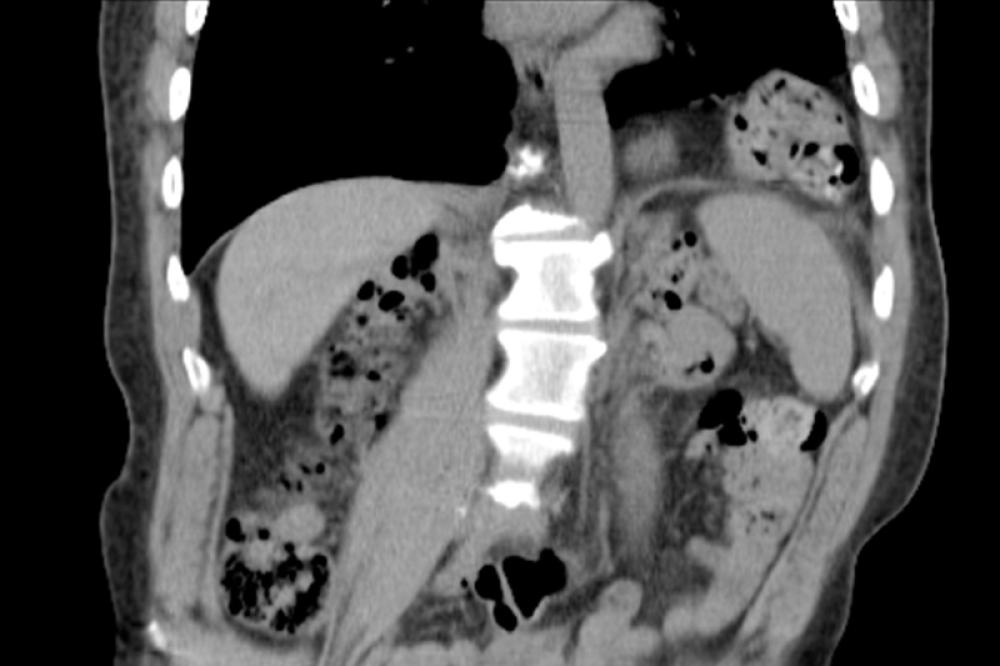
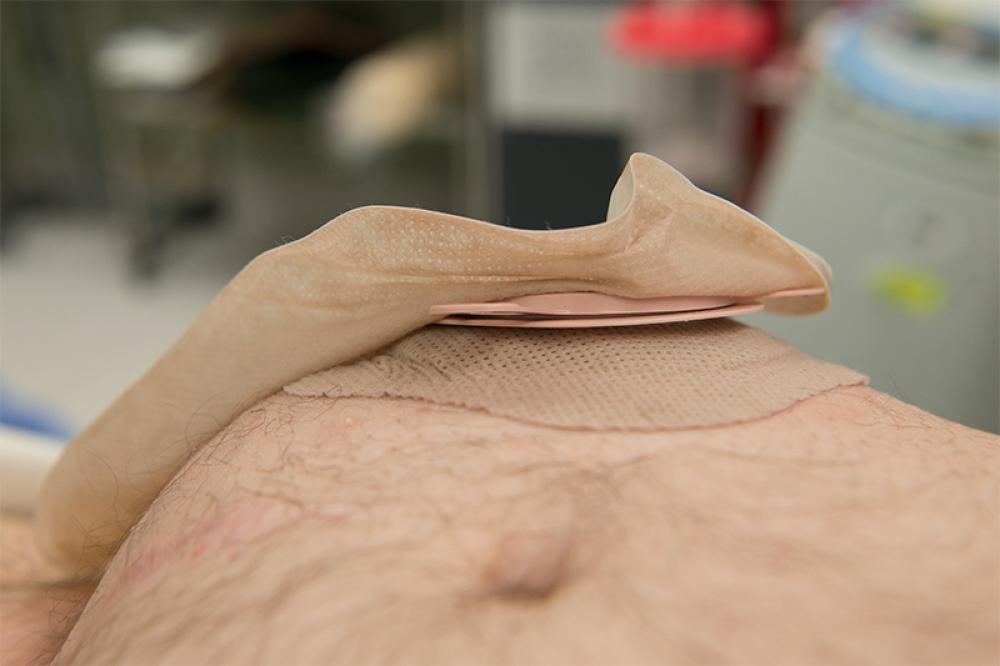
Hernias that occur in the groin are known as inguinal hernias. These are characterized by small balloon-like pouches protruding from the groin region. These form at a natural point of weakness at the intersection of abdominal muscles and are more common in men.
Dr. Belsley's preferred method for fixing groin hernias involves a laparoscopic procedure where he performs the operation inside a natural envelope of muscle outside of your abdominal cavity. This is called a laparoscopic inguinal hernia repair.
Inguinal Hernias travel with the spermatic cord

Groin protrusions occurs when a loop of intestine or fat passes through this a natural weak point and either enters the inguinal canal or pushes out just medial (more in the middle) to the inguinal canal. Men usually suffer from inguinal hernias developing in the groin, and may notice an ambiguous discomfort or even a bulge in the scrotum. Infants and children also suffer from inguinal hernias when a part of the lining of the abdominal cavity called the peritoneum does not close properly. This leads to a bulge in the groin because the intestine or other abdominal contents may push into the opening when the pressures inside the abdomen rise.
Direct Hernia

An example of a hernia bulging outside the abdominal cavity occurs when a patient coughs or has to strain while going to the bathroom. The squeezing that occurs in the abdomen can cause a hernia to protrude. Inguinal hernias can restrict blood supply to the bowel and may cause groin discomfort where there is pain when bending or lifting. Laparoscopic inguinal hernia repair is a surgical repair recommended for inguinal hernias that cause discomfort or for other groin hernias that are enlarging or bothersome.
Laparoscopic inguinal hernia repair is the preferred approach for bilateral inguinal hernia repair compared to open repair. The operation and technique is somewhat similar to other laparoscopic procedures. Laparoscopic inguinal hernia repair must be performed with the patient under general anesthesia. Mesh is required for laparoscopic inguinal hernia repair.
This surgery may not be recommended for those having incarcerated hernias, those with bleeding disorders, nor patients who are too unwell to tolerate general anesthesia. People taking medicines for preventing blood clots, extremely obese persons and pregnant women are more difficult candidates for this surgery. If a patient has had many abdominal surgeries, it can sometimes complicate the laparoscopic hernia approach depending on the location of previous incisions. Scar tissue makes laparoscopic surgery more difficult to perform and optimally a surgeon can select a laparoscopic approach that goes around the scar tissue.
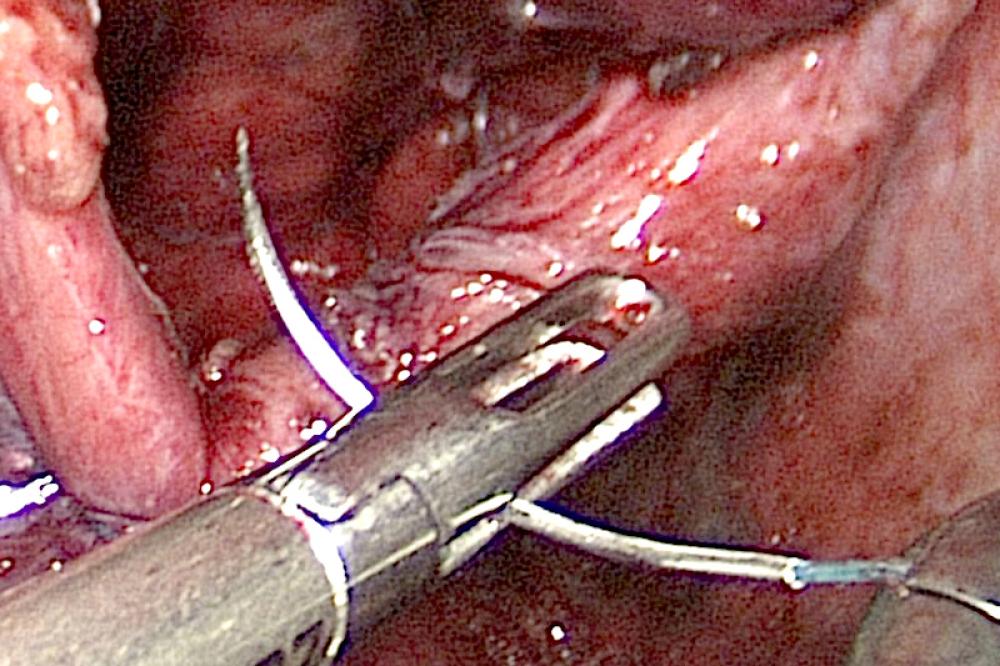
Rolling up and inguinal hernia mesh
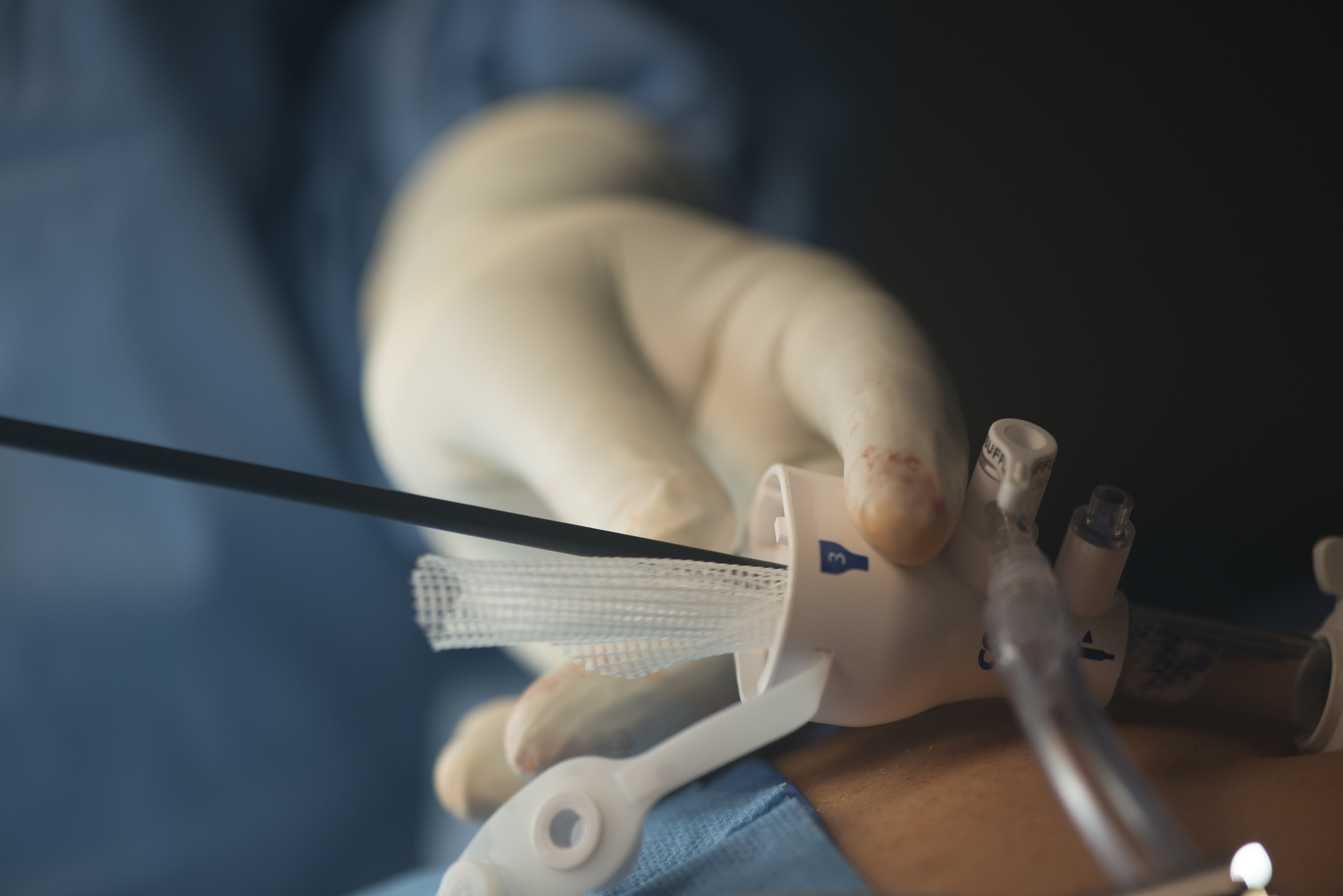
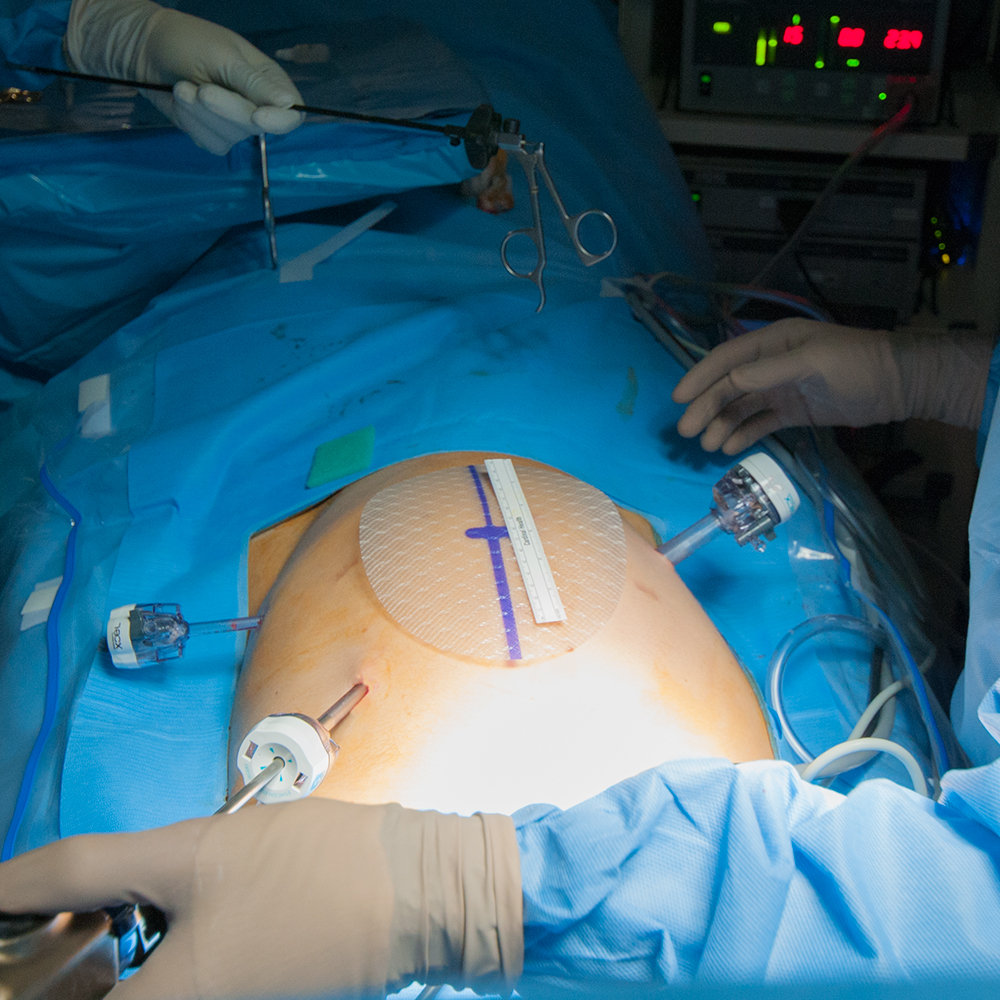
The procedure
A small incision is made in or below the navel and then two additional small incisions are made usually in the midline. A portion of the abdomen wall is inflated with air so that the surgeon can see an operating space. The preferred laparoscopic approach is a TEPP repair which stands for totally extraperitoneal pre-peritoneal repair. The important distinction here is the distinction ‘totally extraperitoneal’. This means that the inside of the abdominal cavity is not filled with air but rather that the air goes between the inside muscle layer and where the hernia is located. The layer of the abdomen just below the muscles is inflated with carbon dioxide and the laparoscope and surgical instruments are inserted through the incisions. With the help of a monitor, the surgeon pushes the herniated abdominal contents into their correct place and then uses a surgical mesh to repair the hernia opening.
Advantages of laparoscopic inguinal hernia repair
The greatest advantage of laparoscopic inguinal hernia repair is that it offers a quicker recovery and thus shorter time off of work than the open repair. You can return home within 24 hours of the surgery and recover within one to two weeks. There is also a reduced risk of infection and the recurrence of hernias with this surgery, leading to less pain than open hernia surgery. The added advantages of laparoscopic inguinal hernia repair over open surgery is that the repair of the hernia may be easier with laparoscopic techniques. The surgeon can also check and repair a second hernia found at the opposite side during the operation. With the small incisions involved in this surgery, people prefer this surgery for cosmetic reasons.
Smaller Incisions used for Laparoscopic Repair
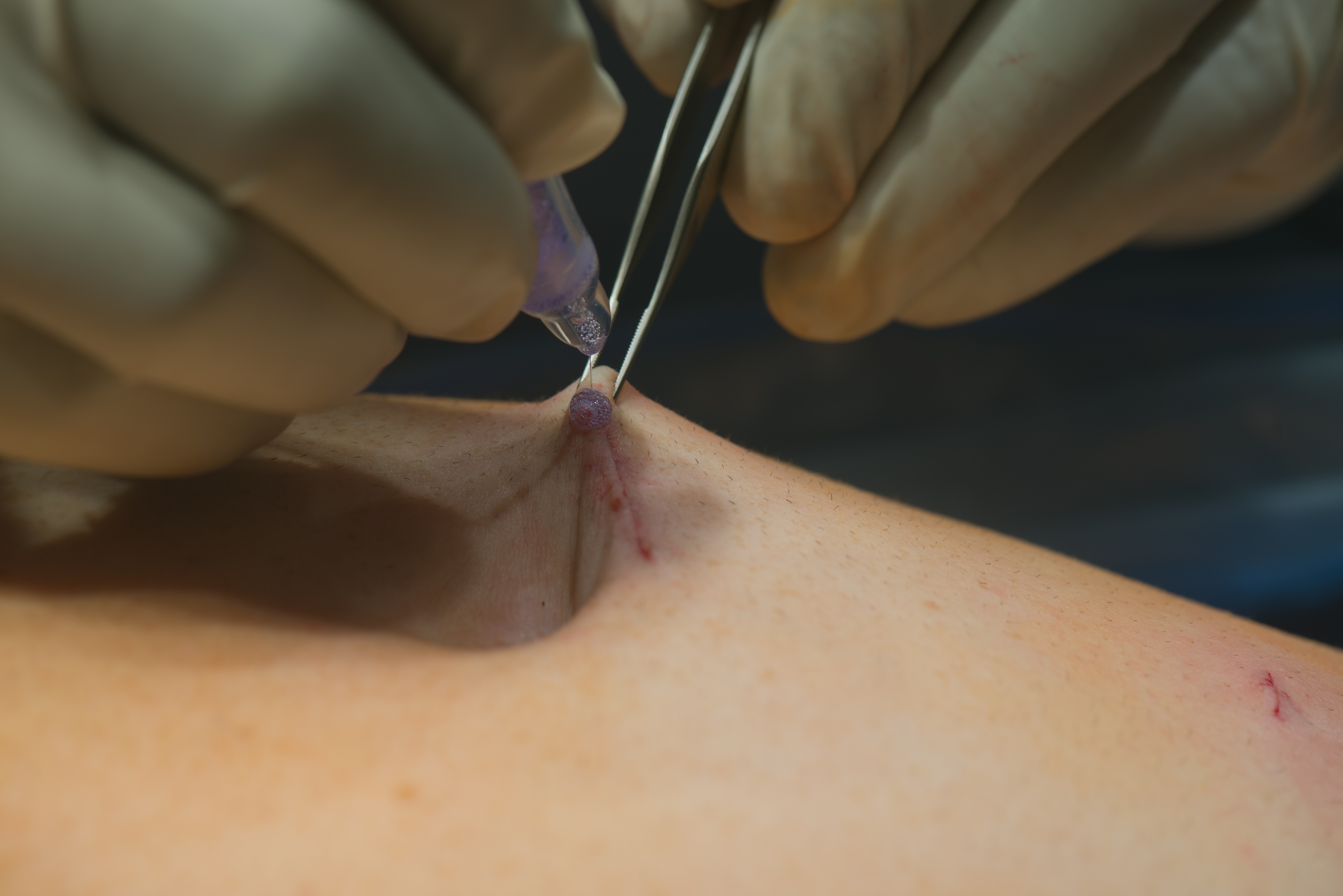
Risks of laparoscopic inguinal hernia repair
Like all surgeries, there are some risks associated with laparoscopic inguinal hernia repair, where some people may need special preparation before the surgery. Those having a history of blood clots in large blood vessels, who smoke and those taking large doses of aspirin (as aspirin slows blood clotting and increases the chances of bleeding with surgery) are most vulnerable. Those on blood thinners and having urinary problems are also not advised the surgery. Some adverse outcomes associated with the surgery include pain in the spermatic cord, presence of fluid or blood in the scrotum and an inabiltiy to urinate. Other complications include from infections from the mesh or stitches, scar tissue formations called adhesions, and an injury to the abdominal organs, nerves and blood vessels. In very few patients, chronic complications include pain in the thigh, an injury to the testicle that leads to testicular atrophy, and a recurrence of the hernia.
Comparing laparoscopic inguinal hernia repair
When compared with open surgery, laparoscopic inguinal hernia repair uses several small incisions instead of a large, single cut. As the surgeon can examine both groin areas, both hernias can be repaired together without any second large incision. With the patch or mesh placed over weak areas of the groin, hernias can be prevented from recurring at the same spot. Theoretically it makes more sense than the open operation because the laparoscopic surgeon does not need to cut through the surrounding muscle layers in order to fix a problem in the same muscle layer. However, laparoscopic inguinal hernia repair is a technically difficult operation. Most doctors would agree that for a one-sided hernia repair- the differences between the open and laparoscopic approach is minimal and depends on your surgeon preference and experience. For operations however that require a bilateral repair (both sides) or if you have previously had a hernia repair and it has come back, then laparoscopic repair is typically preferred.
Bilateral Mesh inside muscle cavity

Dr. Belsley's preferred approach for inguinal hernia repair is laparoscopic repair. All of these operations typically require mesh. Please note that there are patients that may be too obese for hernia repair to occur in any lasting manner. You will be asked your weight and height when calling for an appointment with Dr. Belsley.